Breach Economics
What Does a HIPAA Violation Really Cost You? We Built a Calculator to Find Out.
Discover the real financial impact of HIPAA non-compliance. Use our interactive Breach Cost Calculator to estimate your practice's risk and projected losses.

What Does a HIPAA Violation Really Cost You? We Built a Calculator to Find Out.
When most practice owners think about the cost of a HIPAA violation, they think about fines. The penalty structure is public: $100 to $50,000 per violation, capped at $1.5 million per year per violation category. Those numbers are sobering enough.
But fines are the tip of the iceberg. The real financial impact of a HIPAA violation — especially one that results in a reportable breach — includes costs that most practices never anticipate until they are drowning in them. We built an interactive Breach Cost Calculator to make the full picture visible before a breach forces you to learn it the hard way.
You can access the calculator on our research hub, below the fold. Input your practice size, patient volume, and current safeguards, and the calculator projects your total financial exposure — not just regulatory penalties, but the full cascade of costs that follow a breach.
Why We Built a HIPAA Breach / Violation Calculator
The compliance industry has a communication problem. It talks about HIPAA violations in regulatory language — penalty tiers, violation categories, corrective action plans. That language does not connect with a dentist trying to decide whether to spend $49 per month on compliance software or use that money to repair the compressor.
We built the calculator because the economics need to be concrete. Not theoretical. Not expressed in averages that blend enterprise health systems with solo practitioners. Specific to your practice type, your patient volume, and your current security standing.
The calculator draws on data from OCR enforcement actions, published settlement agreements, industry breach cost studies, and our own analysis published through the Secure Care Research Institute. It is not an estimate — it is a model. And for most independent practices, the output is a number large enough to change the conversation.
The Four Penalty Tiers
HIPAA's penalty structure operates on four tiers based on the level of culpability:
Tier 1 — Did Not Know: The practice was unaware of the violation and could not have reasonably known. Penalties range from $100 to $50,000 per violation. This sounds merciful until you realize that a single breach can involve thousands of individual violations — one per affected patient record.
Tier 2 — Reasonable Cause: The practice should have known but the violation was not due to willful neglect. Penalties range from $1,000 to $50,000 per violation. This is where most under-resourced practices land. They knew compliance was required. They just did not have the infrastructure to execute it.
Tier 3 — Willful Neglect, Corrected: The violation resulted from willful neglect but was corrected within 30 days. Penalties range from $10,000 to $50,000 per violation. OCR considers the absence of a documented compliance program as evidence of willful neglect.
Tier 4 — Willful Neglect, Not Corrected: The worst category. Penalties are a flat $50,000 per violation, up to the annual cap. If you have never conducted a risk assessment and cannot produce documentation of any compliance efforts, you are in Tier 4 territory.
The annual cap is $1.5 million per violation category under OCR enforcement discretion. But there are multiple violation categories, and a single breach can trigger findings across several — meaning the effective cap is substantially higher than most practice owners realize.
What the Calculator Shows You
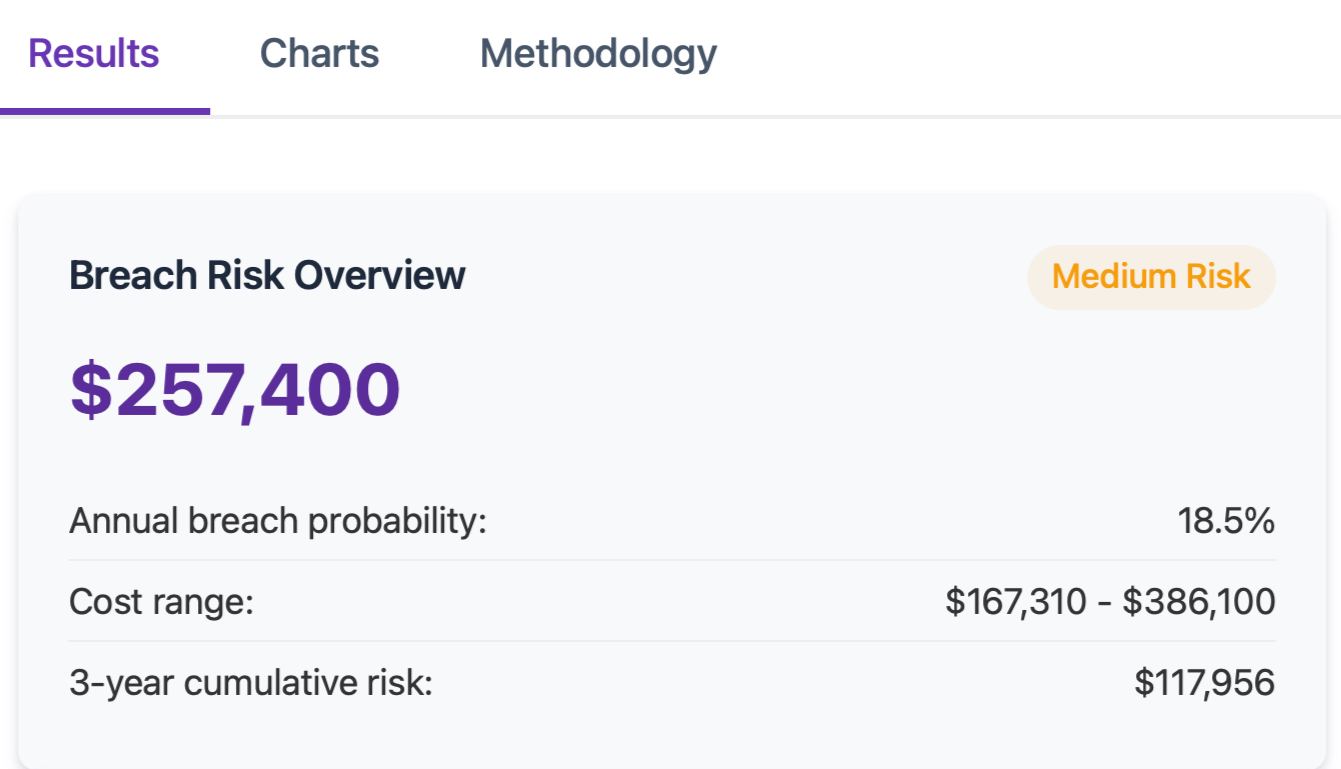
When you input your practice parameters, the calculator produces a projected total cost breakdown across six categories:
Regulatory penalties. Based on your compliance standing, patient volume, and the probable penalty tier, the calculator estimates your likely OCR penalty range.
Forensic investigation. Every reportable breach triggers a forensic investigation. For small practices, this typically costs $75,000 to $250,000 — covering system analysis, evidence preservation, scope determination, and remediation verification.
Legal fees. Breach response requires specialized legal counsel. Attorney fees for HIPAA breach response typically range from $50,000 to $300,000, depending on breach scope and whether litigation follows.
Patient notification and credit monitoring. Federal law requires notification of every affected individual. With costs of $5 to $30 per notification and $10 to $25 per person per year for credit monitoring, a breach affecting 5,000 patients can generate $75,000 to $275,000 in notification and monitoring costs alone.
Revenue loss. During and after a breach, practices experience significant revenue decline. Appointment cancellations during system downtime, patient attrition following breach notification, and reduced new patient acquisition can reduce revenue by 20 to 40 percent for 12 to 24 months.
Reputation and operational recovery. The costs of rebuilding trust, replacing departed staff, implementing corrective actions, and restoring normal operations. These are the hardest to quantify and often the most devastating.
The Costs Nobody Talks About
Beyond the categories in the calculator, there are costs that resist quantification but are no less real.
Cyber insurance premium escalation. After a breach, practices face premium increases of 200 to 400 percent — if coverage is renewed at all. Some carriers now refuse to underwrite practices with prior breach history.
Personal liability exposure. Practice owners can face personal liability for HIPAA violations, particularly when OCR determines that leadership failed to implement required safeguards. State attorneys general can pursue individuals, not just entities.
Emotional and psychological toll. Breach response is grueling. The investigation disrupts every aspect of practice operations. Staff morale collapses. The practice owner — who went into healthcare to help people — is suddenly managing a legal and regulatory crisis instead of treating patients.
Competitive disadvantage. Practices that appear on the HHS breach portal face permanent reputational damage in their local market. Competitors reference the breach. Patients reference the breach. The stigma does not expire.
Healthcare breaches cost $9.8 million on average — the highest of any industry for fourteen consecutive years. For independent practices, the relative impact is even more severe. A practice generating $800,000 in annual revenue cannot absorb a $2.8 million breach cost. The economics of breach exposure for small practices are existential, not inconvenient.
The Calculation That Should Change Your Mind
Run the calculator on our research hub. Input your actual numbers. Look at the output.
Then compare that number to the cost of active compliance. Patient Protect starts at $39 per month. That is $468 per year for a platform that satisfies 25 HIPAA requirements automatically, provides continuous monitoring, and delivers the documentation you need to demonstrate compliance during an audit or investigation.
The risk-adjusted return is not subtle. It is one of the clearest investment decisions in healthcare operations.
If you are not ready to commit to a platform, start with the free tools. The risk assessment identifies your current exposure. The breach dashboard shows you the live threat landscape. The Patient Protect Signal app delivers breach alerts and compliance tools directly to your phone.
The cost of a HIPAA violation is not what you think it is. It is worse. The calculator proves it.
