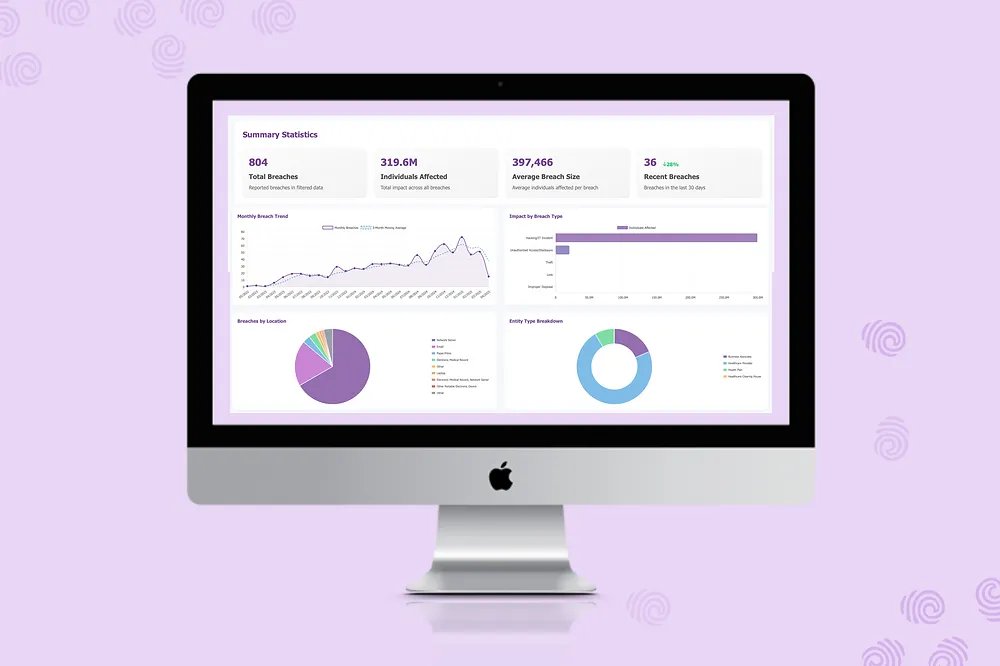
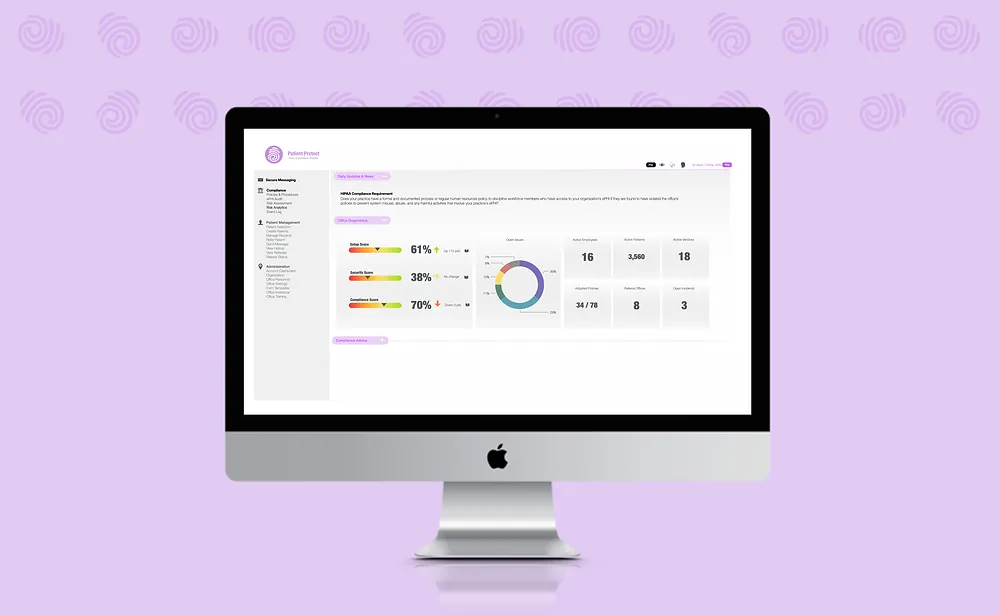
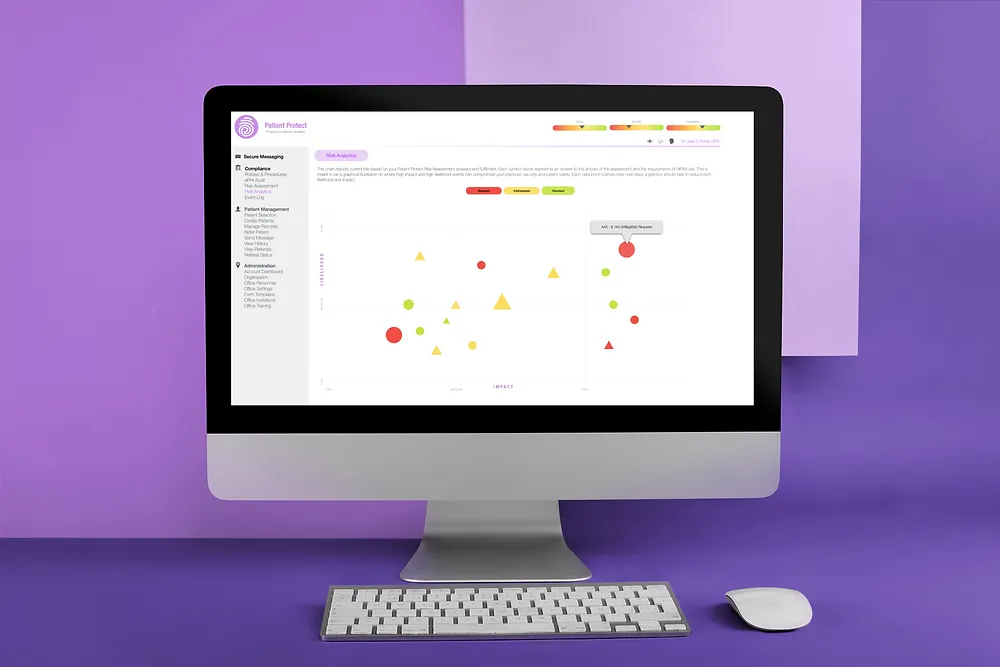
Healthcare Data Breach Statistics 2026: 190M Patients, $9.8M Per Breach
276 million Americans had health data exposed in 2024. Medical records sell for 10x the value of credit cards. AI amplified exploit value by up to 30%. Here are the numbers — and what they mean.